Dr Fabienne Marchand-Lamiraud
Pathophysiological data, clinical indications and clinical experience feedback.
Platelet-rich plasma (PRP) has been used for many years in in various therapeutic fields and produces good results. However, its application in gynaecology is quite recent and little known, but is currently being developed, particularly in the treatment of lichen sclerosus (LS).
What is platelet-rich plasma?

The plasma obtained after a centrifugation, with a specific protocol, of a blood sample is rich in platelets. These platelets, whose role in hemostasis is well known, provide essential growth factors. These play a role in stem cell multiplication and stimulate fibroblasts, which then release collagen (mucosal density and thickness), elastin (tissue suppleness), and hyaluronic acid (hydration), while promoting neovascularisation [1-2].
There are numerous indications for PRP in GYNAECOLOGY
Vulvovaginal dryness and atrophy, lichen sclerosus, obstetric or surgical perineal scars, vulvodynia (particularly idiopathic), mild urinary incontinence, fertility (ovaries, endometrium).
Lichen sclerosus, or vulvar lichen, is a chronic inflammatory disease that causes progressive lesions of the vulva, vaginal opening, perineum, and anal region, with intense functional repercussions. Sometimes, LS is asymptomatic and diagnosed during a routine consultation [3]. LS can affect women of any age, but it is mainly seen in postmenopausal women. However, there are cases in young girls, referred to as lichen pubertalis, and in young children, referred to as pediatric lichen. In these cases, LS tends to worsen during menopause. The disease progresses in alternating phases of recurrence and remission. However, the later ASL begins (after the age of 70), the fewer phases of remission there will be. The risk of cancerisation is significant, occurring in 6% of cases, leading to differentiated vulvar intraepithelial neoplasia or squamous cell carcinoma. This neoplastic progression occurs mainly in cases of poor compliance with topical corticosteroid treatment [4].
Treatments for lichen sclerosus

Treatment is essential to slow the progression of the disease and must not be interrupted in order to prevent recurrence or cancerisation. The standard treatment is the use of topical corticosteroids (clobetasol 0.05%) in initial doses, followed by maintenance doses, with regular medical follow-up. This treatment reduces clinical symptoms, particularly itching and pain, and slows the progression of the disease, but it cannot cure it or regenerate the affected tissue. This is why other therapies have recently been proposed.
My personal experience over 2 years
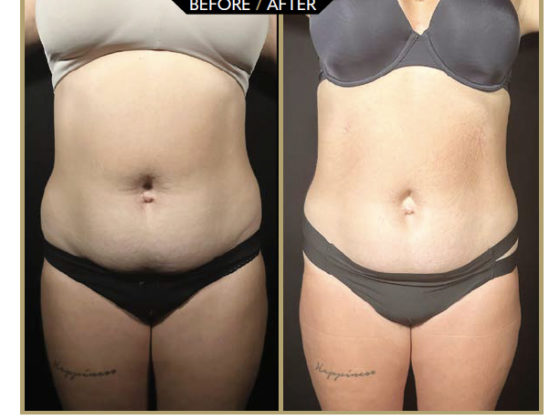
I treated 77 patients between January 2024 and December 2025, performing more than 230 vulvar PRP injections. Each patient received two to three PRP injections at one-month intervals, depending on the severity of the vulvar condition. Some patients required four or even five injections if the lichen was extensive, long-standing and progressive. In 2024, out of 28 patients, 19 experienced a rapid and significant improvement in pruritus, burning and vulvar pain, i.e. 67.8%. All noticed an improvement in tissue suppleness and plumping of the vulva, particularly the labia minora. Sexual intercourse became less painful and then even painless. In 2025, out of 49 patients treated, 33 had the same results, i.e. 67.34%. Many of the patients treated were able to ride a bicycle again and dress without restriction (tight trousers, certain types of underwear, etc.). They say they have regained their femininity and self-confidence and are happy to be able to live freely again without thinking about their vulva! Those who had a painful episiotomy in addition to their lichen saw the scar pain disappear, and 5 patients with lichen sclerosus undergoing hormone therapy for breast cancer saw a clear clinical improvement.
Of these 55 highly satisfied patients, 12 stated during the 6-month telephone call that they had stopped applying topical corticosteroids 1 month after the last injection, and 10 were still not using them 1 year later, reflecting the regression of the disease as shown by photos taken at 1-year and 18-month intervals. Five patients in 2024 and nine in 2025, i.e. 14 patients, saw less dramatic improvement (18%) but reduced the frequency of topical corticosteroid use. Patients who used them daily now only use them once or twice a week or only during flare-ups. Four patients in 2024 and seven in 2025 (14%) saw virtually no improvement except for a feeling of improved tissue suppleness, and the photos taken show no visual improvement in the lichen but also no worsening at two years. We can therefore see that of the 77 patients, 86% experienced a significant improvement with a regression of the clinical signs of lichen, a resumption of their sex life for most of them, and a return to their daily quality of life, with either a cessation of topical corticosteroids or a reduction in the frequency of application.
PRP is a major breakthrough that greatly improves women’s quality of life in their daily lives and sexuality. PRP is of particular interest in LSA because it stops the progression of the disease, causes it to regress and therefore reduces the risk of cancerisation. L
References
1. Fountain JH, Lappin SL. Physiology, Platelet. Treasure Island (Fl): StatPearls publishing, 2025.
2. Joscilin M et al. Physiology, Blood plasma. Treasure Island (FL): StatPearls publishing, 2025.
3. De Luca DA et al. Lichen sclerosus; the 2023 update, FrontMed (Lausanne), 2023;10:1106318,
4. Halonen P etal. Lichen sclerosus ‘and risk of cancer. Int | Cancer 2017;140(9):1998-2002
Dr Fabienne Marchand-Lamiraud

Gynaecological Surgeon, Intimate Reconstructive Medicine and Surgery, Aesthetic Medicine. Elsan Santé Atlantique, Nantes.Graduate of the Paris Créteil Faculty of Medicine in Aesthetic Gynaecology (CUMEG). Member of AMME and AFME.